Ptosis in Myasthenia Gravis

To download a peer-reviewed article on ptosis in patients with myasthenia gravis (includes ocular myasthenia gravis) by Prof BCK Patel MD, FRCS & team published in the british journal of ophthalmology, please download here
Important
What is myasthenia gravis?
myasthenia gravis is from the Greek myasthenia (muscle weakness), and the latin word gravis (serious).
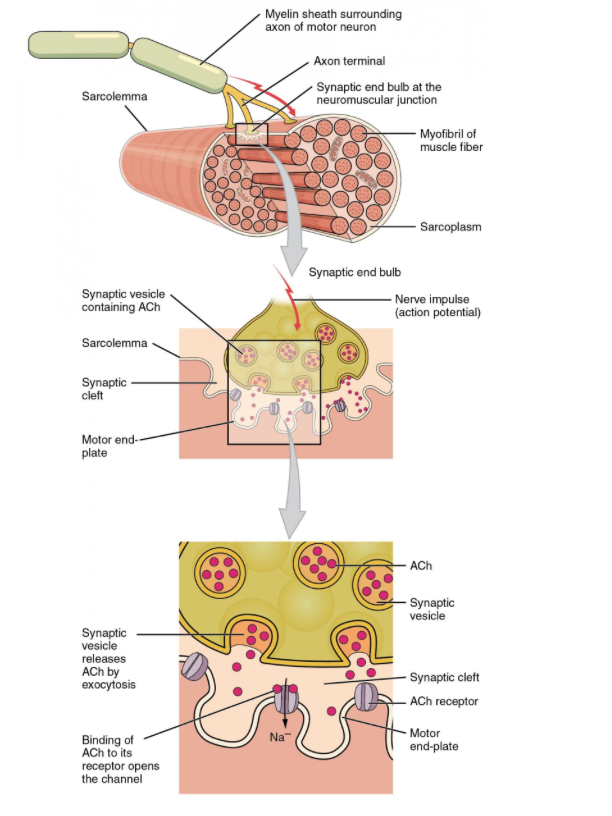
Myasthenia Gravis (MG) is an autoimmune disease: postsynaptic acetylcholine receptors at the neuromuscular junction of skeletal muscles are targeted: the result is muscle weakness which shows fatigability. Blocking of neuromuscular transmission occurs, causing the muscle weakness.
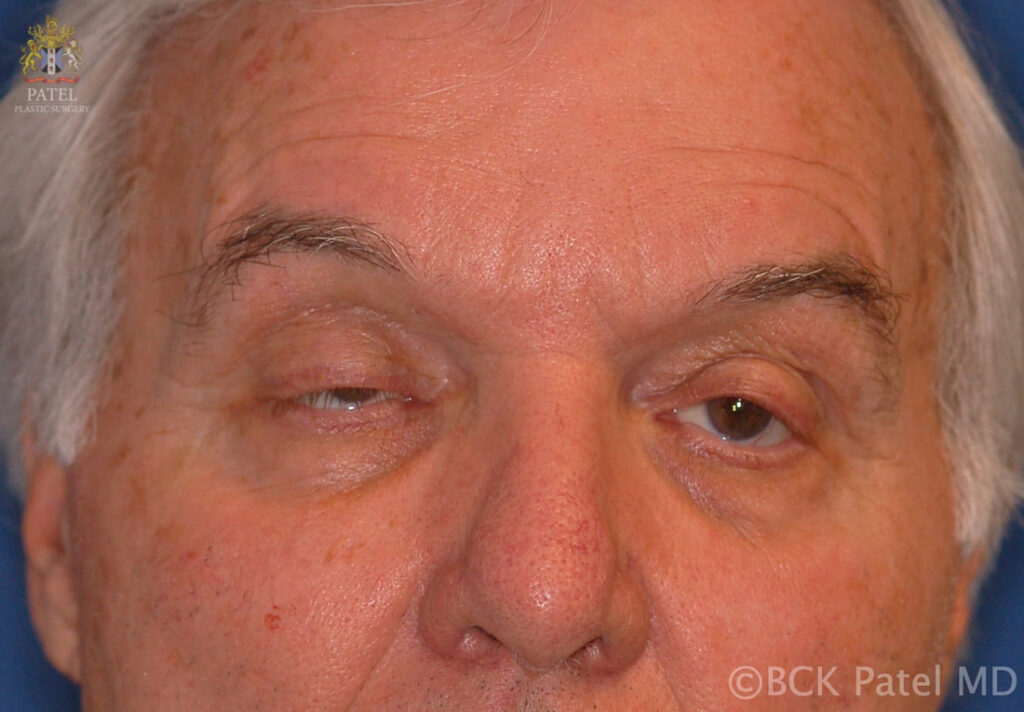
how does myasthenia gravis present?
The disease essentially presents with muscle weakness which worsens with muscle use (the muscles fatigue). The symptoms are generally worse later in the day for that reason.
- At initial presentation, more than 50% of patients will have ocular symptosms (droopy upper lids – ptosis, or double vision because of the involvement of the extraocular muscles
- Nearly 90% of patients with myasthenia gravis have eventual involvement of the ocular muscles
- Approximately 50% of patients who are seen with initial ocular weakness will develop generalized weakness within 3 years of initial presentation
- About 25% of patients will only have ocular findings and no generalized muscle weakness. There is a thought that over time, this number decreases
- About 5% of patients present initially with limb weakness (proximal is more severe than distal)
- It is common to undergo exacerbations so that the weakness my vary from ile to severe over time
- Difficulty in swallowing, slurred speech, chewing difficulty, facial weakness
- Muscle weakness is worsened by activity and improves with rest. Hence the droopy upper lids are better in the morning or after sleep
He treated us as friends
Parents of child with Blepharophimosis Syndrome, USA
Fortunately, for us, Dr. Patel at Primary Children’s Hospital – Moran Eye Center, was equally comforting as he was qualified. He has phenomenal bedside manners, and is an extremely kind human being. Nothing about our experience with him made us feel like he was in a routine, or that he’d seen this a thousand times, he treated us as friends, and as if he was bearing this burden with us.
What factors may worsen symptoms in myasthenia gravis?
- heat (warm weather)
- trauma (emotional stress, surgery, illness)
- menstruation
- pregnancy
- a number of medications
Dimitry, also in 1921, coined the term “Blepharophimosis” when de described a family with the condition and he was the first to note the dominant inheritance of this condition.
how is myasthenia gravis diagnosed?
- Anti-acetylcholine receptor antibody test is highly specific and is positive in up to 85% of patients who have generalized weakness. However, only 50% of patients with only ocular myasthenia will have a positive result
- False positive anti-acetylcholine receptor antibody results may be seen in patients with thymoma without MG, small lung cell cancer, rheumatoid arthritis, Lambert-Eaton syndrome and up to 3% of people older than 70 years
- Other tests for MG include anti-MuSK antibody test, anti-lipoprotein-related protein 4 antibody (LRP4), anti-agrin antibody, antistriational antibody and anti-cortactin antibody
- Chest X-rays may show a thymoma (anterior chest mass)
- All patients need a chest CT looking for a thymoma or thymic enlargement
- Single-fiber electromyography
- Edrophonium (tensilon) is a short-acting AChE inhibitor that improves muscle weakness in patients with MG.
- Ice Pack Test: place ice over the closed eyelid. Improvement in the ptosis and/or diplopia may be seen. This may be because of the cooling or because of the resting of the eyelids!
- Cogan sign. The patient is asked to look from down to straight ahead. The upper lids over-correct and then settle
clinical assessment of myasthenia gravis
- The ptosis can be shown to worsen if the patient is asked to sustain an up-gaze for two to three minutes
- The Herrings Law is “more significantly positive” in patients with MG
- “The Peek Sign”: sustained squeezing of the eyelids (orbicularis oculi muscle) will show weakening and the sclera will become visible with the eyelids partially open
- By sustaining lateral gaze, diplopia may be elicited
- Arm weakness may be apparent by sustained abduction of the arms (arms held out away from the body)
- Patients with involvement of the nasal and lingual muscles will show fatiging when counting aloud from 1 to 50
- Patient unable to keep the leg raised whilst lying down
- Repeated standing from a chair will show fatiguing
- Hyperthyroidism is seen in up to 15% of patients with MG (more commonly seen with ocular MG) and treatment of one does not improve the other disease
My eyes are so much more comfortable now
W.E 53 Yrs Old with "trouble until I came here!"
Why don’t we have more doctors like this doctor? He really knows his stuff but he is also very patient and explains things clearly.
I had botched surgery and had too many operations (five). Every time someone would see me they would want to operate and I was always left worse off. I finally was very frustrated and did not want to come from Montana and drive 8 hours just to see yet another doctor but I am so glad I did. My eyes are so much more comfortable now after Dr. Patel’s care and I even look better. He took his time analyzing all my procedures and planning things and I will always be grateful to him and to the University for having this great doctor.
Billings, MT
management of myasthenia gravis
There has been impressive progress in the management of myasthenia gravis as we now understand that therapy may be focused based upon a number of factors, including the different antibodies involved, the differences in clinical presentation, the age of onset, presence or absence of thymic involvement, and the weakness distribution.
A brief summary of management is as follows (careful assessment and treatment are by neurologists or neuromuscular specialists):
- Anticholinesterase inhibitors with pyridostigmine for maintenance treatment (neostigmine is used when pyridostigmine is not available)
- Intravenous immune globulin
- Prednisone as an immunosuppressive agent for long-term maintenance therapy
- Azathioprine may be used as a steroid-sparing agent
- Mycophenolate mofetil has been found to also be steroid-sparing and less toxic than azathioprine
- Cyclosporine. Methotrexate and Tacrolimus are other steroid-sparing agents
- Rituximab has been found to be effective in refractory MG
- Cyclophosphamide is used in severe or refractory MG
- There are a number of newer monoclonal antibodies that are being tested and hold much promis
- It has been shown that a thymectomy improves MG and may reduce or eliminate the need for systemic medication. All patients with myasthenia gravis are worked up for involvement of the thymus and considered for a thymectomy
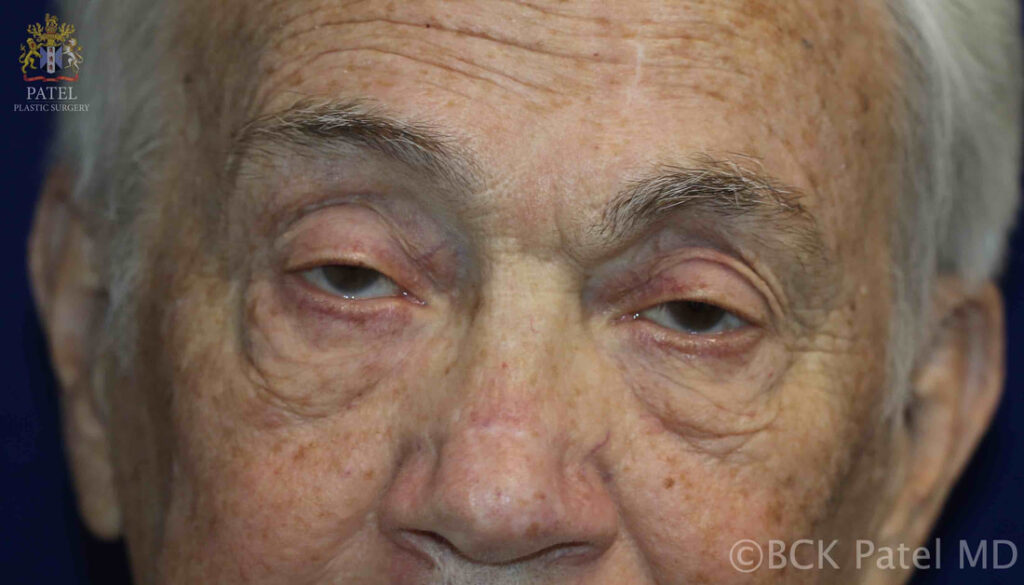
what are the ocular findings in myasthenia gravis?
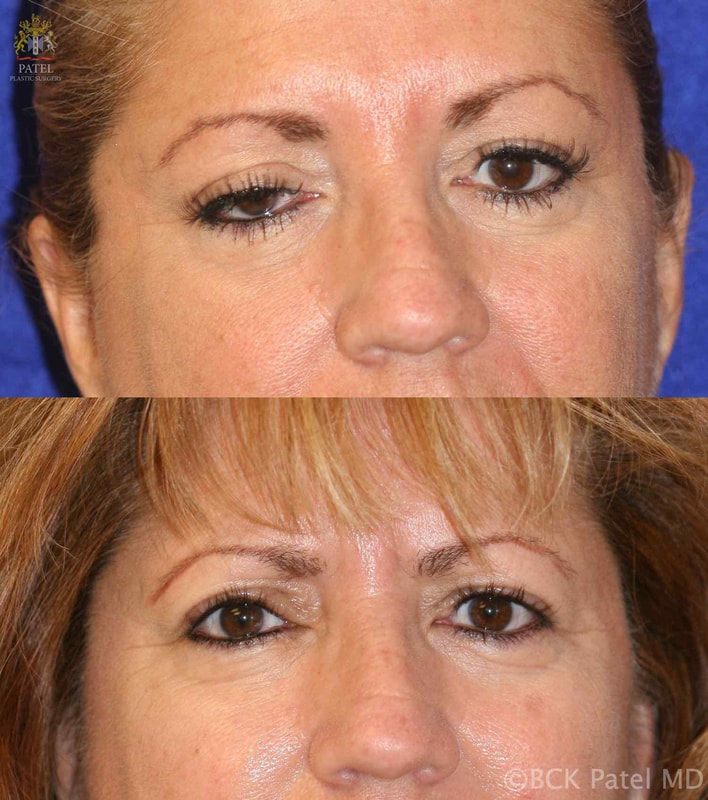
As mentioned, ptosis and double vision are common and over time, more than 90% of patients with MG will demonstrate ocular findings. The ptosis is minimal early in the morning and worsens through the day. The ptosis may be asymmetric.
Double vision may be intermittent of constant. Initially, patients may present with just blurred vision. Pupil function in MG is always normal.
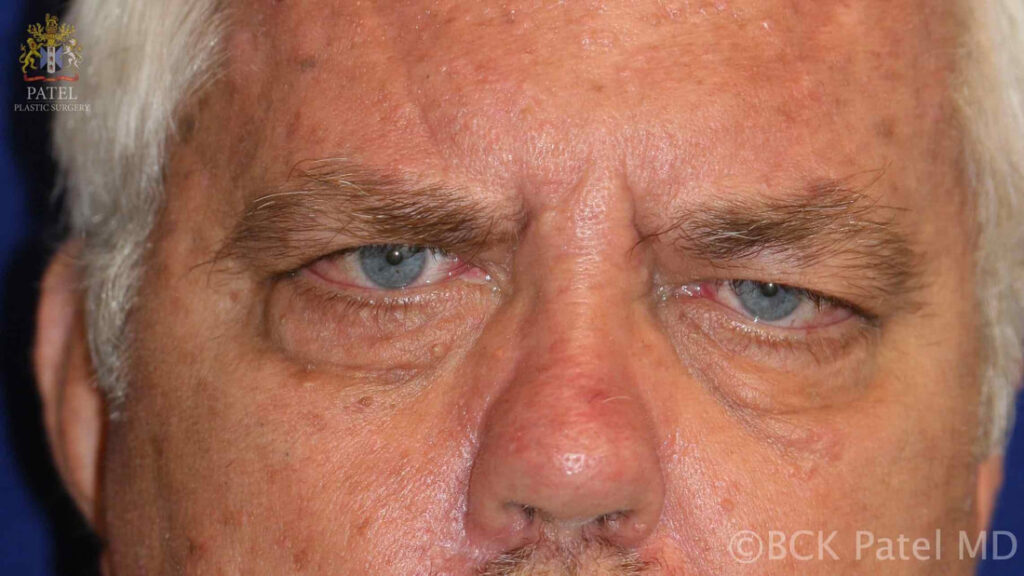
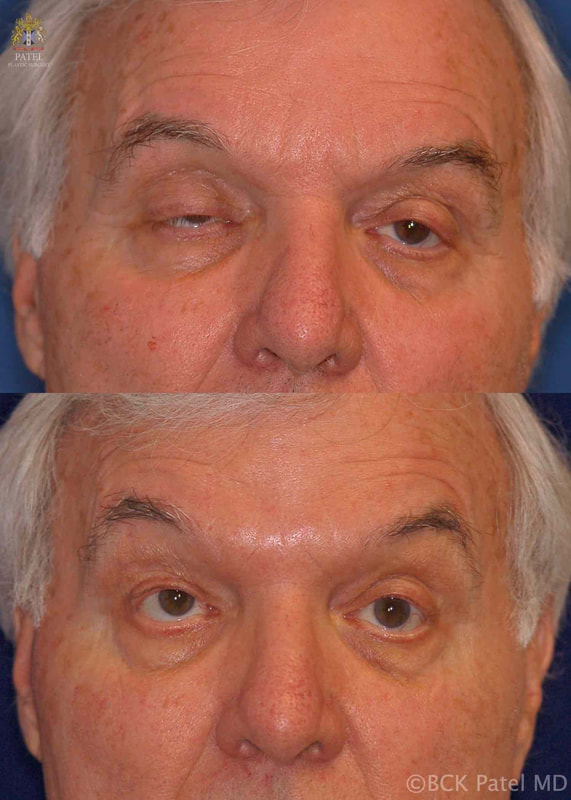
Assessment of Ptosis in myasthenia gravis
Ptosis repair requires careful assessment of patients with myasthenia gravis because of a number of other factors that may affect the choice and procedure for ptosis correction. Specifically,
- The Bell’s phenomenon may be weak or neutral or negative
- Weakness of the orbicularis muscle can result in increased dryness and exposure (lagophthalmos)
- Incomplete blink
- Infrequent blinking
- Photosensitivity, which is present more often in such patients
- Variable ptosis with variable measurements of levator function
Ptosis repair in myasthenia gravis
In a comprehensive review of patients we repaired and followed, we have shown the following:
- Complete ptosis correction is inadvisable: aim to lift the eyelid to a functionally useful level without creating excessive corneal exposure, dryness and photophobia
- Patients with severe ptosis will still show impressive levator function: this can fool the surgeon into performing excessively aggressive surgery
- Expect the lid height to decrease over time
- Frontalis slings may be indicated sooner than with patients with severe ptosis but without MG
- When placing slings, use reversible materials as adjustments may be necessary
- When placing slings, aim to allow the lids to close gently but completely when the brows are relaxed. This is contrary to what is done when inserting slings for severe ptosis in patients without MG
- Be conservative with resection of skin and orbicularis muscle in patients with MG
- Beware the lower eyelids: lower eyelid laxity or retraction are not uncommon and are often missed. We always measure the lower lid tone and position and correct any laxity or retraction so as to allow for successful ptosis surgery
- Double vision should not be treated with surgery. It will improve with medical treatment of patients with MG
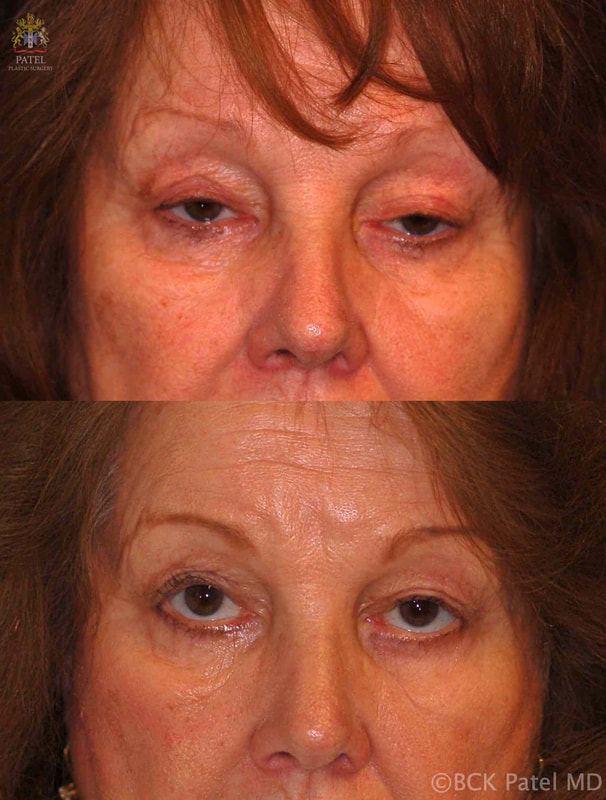
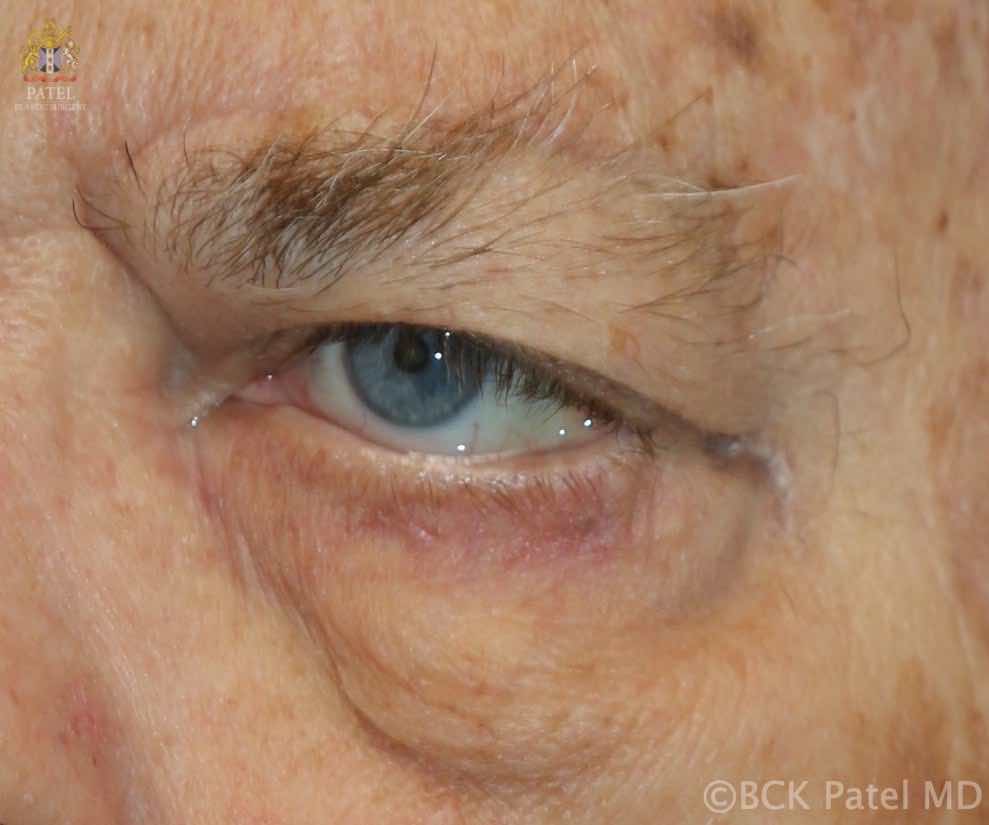
Highly recommended for eye lift surgery
Salt Lake City, UT
I had a excellent eye lift done by Dr. Patel. He knows what he is doing and is very pleasant. Dr.Patel was easy to get an appointment and he works with you. The office staff was very pleasant and made you feel calm.
D. Gull
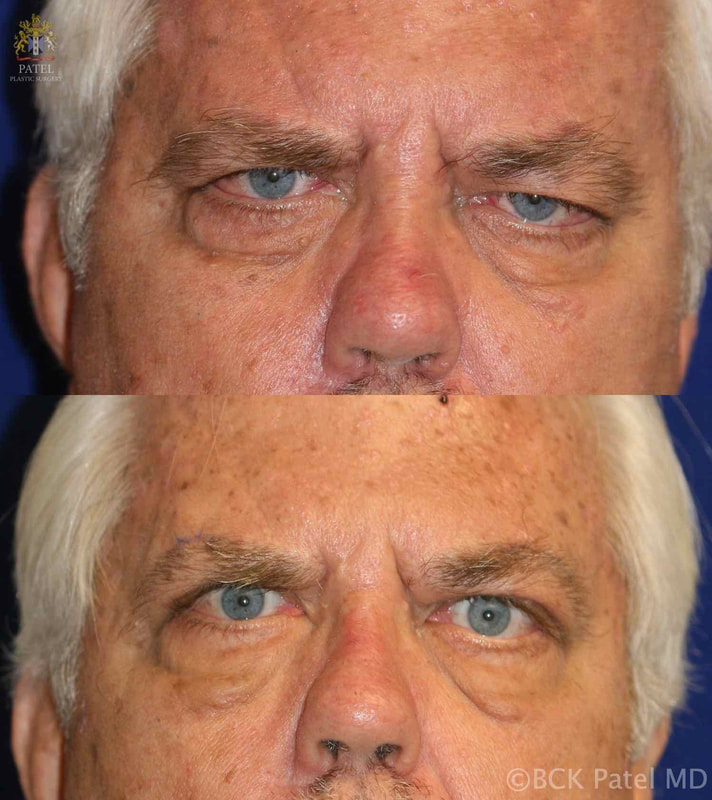
Brow ptosis in myasthenia gravis
Because of facial muscle weakness, some patients will develop severe forehead (frontalis muscle weakness) and brow droop with secondary dermatochalasis and difficulty with vision.
Such patients need elevation of the brows.
- So-called internal browlifts will not work and are not recommended
- A direct brow lift may be performed
- We designed and presented a form of a mid-forehead brow lift which allows us to improve the forehead and brows with excellent results functionally and cosmetically
- Endoscopic brow lifts which we use in cosmetic brow elevation will not work long-term in patients with MG
- String-browlifts, suture-browlifts and other minimally invasive techniques will not work in patinets with MG
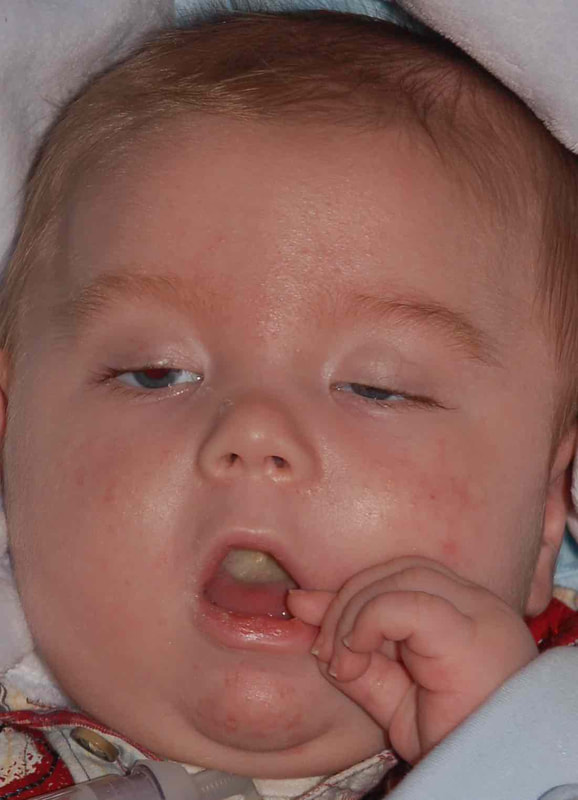
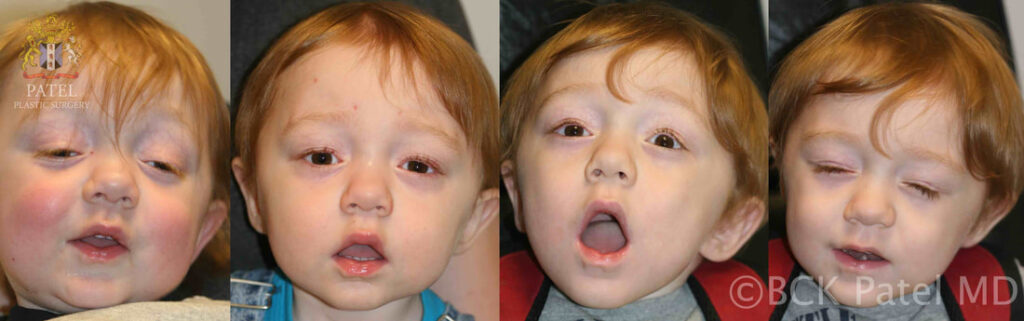
myasthenia gravis in children
Myasthenia gravis may be seen in newborns when the mother is affected by MG. The MG here is transient. Only about 20% of infants born to mothers with MG will develop neonatal MG.
If MG persists, then treatment of the droopy upper lids is needed.
care of upper eyelids after ptosis Surgery
Some degree of difficulty closing the eyelids for the first few days is normal and to be expected.
After surgery, the following instructions should be followed:
- The incision sites will need the application of erythromycin eye ointment three times a day for about a week: this will be prescribed.
- It will be important to keep the incision sites clean: clean hands!
- Any oral antibiotics prescribed (especially important when frontalis slings are performed) must be administered.
- For the first few weeks, applying a small amount of eye lubricating ointment (Refresh pm ointment or any other eye lubricating ointment will do) whenever one naps or sleeps at night. After a few weeks, most people do not need continued application of ointment unless one is unwell (colds, illness, etc)
- The sutures dissolve over two weeks.
- During the day, lubrication with artificial tears may be needed for the first few weeks.
What sort of scars will there be?
When a direct incision is made to lift the eyelid, the incision is hidden in where a natural crease would form. Scars may have a few bumps (because of the deep sutures), but these disappear over time.
After frontalis slings, the incisions become almost invisible within a few months as we make very small incisions using a technique that we developed at the University of Utah and have taught to surgeons from all over the world. We take pride in our “small-incision” frontalis slings with minimal scars, unlike the way the surgery is performed in many other centers. It is normal to feel small bumps under the skin after frontalis slings as the sling material is attached to the frontalis muscle: however, these are rarely visible.